The Endurance Athlete's Guide to Hormonal Contraceptives

(Photo: Getty Images)
“Female athletes are often neglected in exercise physiological research.” This phrase, or some variation of it, is something you read often when trying to get a clear understanding of how something like birth control affects triathletes.
The lack of information is especially frustrating when you consider that approximately half of athletes who menstruate are using a hormonal contraceptive. In a political climate that is increasing restrictions around reproductive health care, it is even more imperative that people who menstruate are given clear information about how different birth control methods could affect their bodies.
But there’s the rub: female athletes are often neglected in exercise physiological research. Though the field is growing, definitive scientific evidence on how hormonal contraceptives affect runners, triathletes, and other endurance athletes is a work in progress. Get ready for a lot of “mays” and “mights” and “potentiallys” as we ask the experts to break down how hormonal birth control affects endurance athletes.
RELATED: The Gender Gap in Sport Research is Holding Female Endurance Athletes Back
First: What Are Hormonal Contraceptives?
Hormonal birth control comes in a wide array of brands, types, and formulations. In total there are nearly 200 variations of birth control on the market today.
Based on your needs and lifestyle, doctors will prescribe combined estrogen and progestin pills or progestin-only pills, injections, implants, intrauterine devices (IUDs), or patches. The most common type of hormonal contraceptive, however, is the combination pill containing estrogen and progesterone.
How hormonal contraceptives work
Hormonal contraceptives (HCs) are made up of synthetic hormones that mirror the natural ones in the female body. They work to override the menstrual cycle.
The progestins and estrogens in hormonal contraceptives signal the pituitary gland to not produce follicle stimulating hormone (FSH) and luteinizing hormone (LH), effectively suppressing ovulation.
When administered properly, HCs are very effective at preventing pregnancy.
Types of hormonal contraceptives
| Type | Hormones | Effectiveness (w/ correct use) | Possible Side Effects |
| Implant (Nexplanon) | Progestin | 99% | Irregular bleeding in first 6-12 months Loss of period Headaches Breast Pain Nausea |
| Hormonal Intrauterine Device (IUD) | Progestin | 99% | Cramping for a few days after insertion Irregular bleeding Loss of period |
| Depo-provera shot | Progestin | 96% | Irregular bleeding Loss of period Nausea Weight gain Headaches Sore breasts Depression |
| Birth control ring | Estrogen & Progestin | 93% | Headaches Nausea Sore breasts |
| Birth control patch | Estrogen & Progestin | 93% | Headaches Nausea Sore breasts Changes to menstruation Skin reactions at site |
| Combination pills | Estrogen & Progestin | 93% | Nausea Blood clots High blood pressure |
| Mini pills | Progestin | 93% | Headaches Nausea |
Uses of hormonal birth control
The main use for hormonal contraceptives is to prevent pregnancy, but there are other health reasons why a person may be prescribed a contraceptive. If you have pain or irregularity surrounding menstruation, for example. Using birth control can also manage the menstrual cycle, helping to keep hormones stable to minimize changes in performance. Or menstrual bleeding can be eliminated entirely, adding a bit more convenience to the athlete’s life (though this might not be advisable for endurance athletes as it can mask symptoms of overtraining). Hormonal birth control can help manage premenstrual syndrome, improve acne, and may reduce instances of migraine. It can also lower the risk of ovarian cancer, uterine cancer, and colon cancer, while slightly increasing the risk of breast cancer. It can be used to treat Polycystic Ovarian Syndrome (PCOS), endometriosis, and uterine fibroids.
Low-dose pills can also be prescribed to treat the symptoms of perimenopause, like hot flashes or irregular periods.
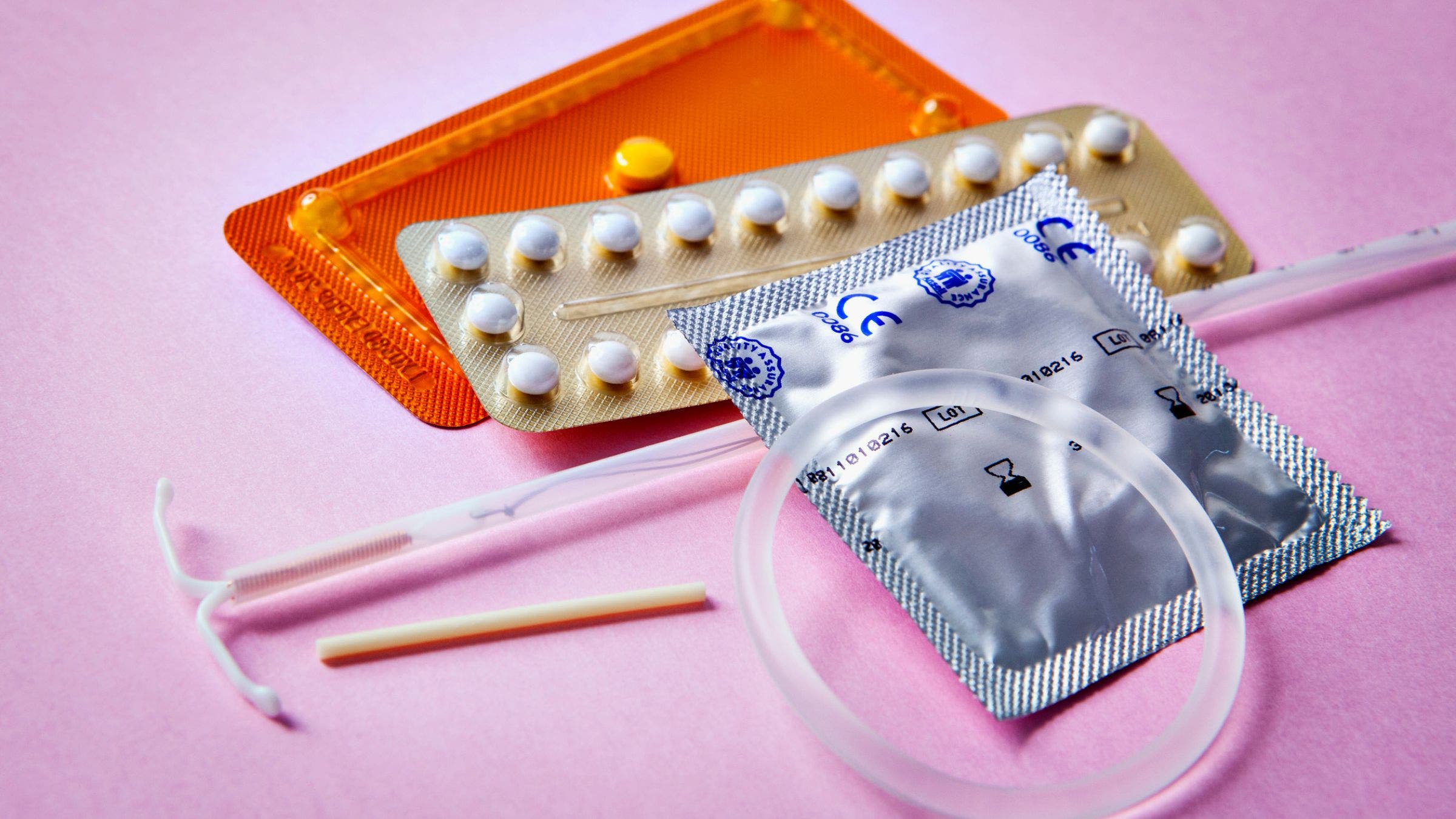
How does hormonal birth control affect me as an athlete?
There is still so much research that needs to be done on female athletes and birth control. But we’ll break it down the best we can based on the research that is out there.
Hormones are pretty variable from person to person. Some women have a larger concentration of hormones in the blood, and are therefore more susceptible to physiological changes that come with that. And with any medication, there comes a list of side effects that you may or may not experience (with HCs that could be an increased number of headaches, nausea, cramping, depression, etc.).
Understanding how hormonal contraceptives affect athletic ability is challenging too because different types of birth control use different hormones, and often in studies–especially older studies–all birth control users are lumped together.
General side effects
Studies show that a large portion of female athletes experience side effects from either hormonal contraceptives or their menstrual cycle. And it can be assumed that negative side effects like migraine, headaches, cramping, and fatigue will have an effect on endurance performance.
In a paper published in 2022 that surveyed over 1,000 athletes from 57 sports, 47 percent of oral contraceptive users reported a negative impact to their performance in the inactive week of their pill regimen. The subjective impact was reported as affecting their physical and mental ability as well as their sleep.
But the big question athletes want to know is ‘will this affect my swim, bike, and run?’ The very general answer is, probably not.
One meta-analysis of 42 different studies found that menstruating athletes taking oral contraceptives did experience a performance deficit in comparison to naturally menstruating athletes, but that deficit was small enough to be deemed insignificant. In the end, the authors recommended that the effects of contraceptives be considered on an individual basis.
And some cases have shown a small reduction in VO2 Max, by 2-4 percent, a difference that is probably negligible to a recreational triathlete.
Ritva Mikkonen, Ph.D., an exercise physiology researcher, notes that “on average, we can say that hormonal contraceptives do not significantly affect training adaptations, but on an individual level there is variation that could be meaningful for an athlete.” Which is why she is quick to recommend that all female athletes track their menstrual and hormonal birth control cycles to detect personal patterns.
RELATED: Period Tracking for Female Athletes
On average, we can say that hormonal contraceptives do not significantly affect training adaptations, but on an individual level there is variation that could be meaningful for an athlete.
Hormonal birth control and athletes: Effects on strength
A 2021 study published in the Journal of Strength and Conditioning Research, has been highly circulated for its results regarding muscle gains, but like with many of the studies out there, it’s important to note the small sample size: 38 natural cycle women and 34 on oral contraceptives. The study, which followed a 10-week resistance training program measuring body composition and looking at blood samples before and after training, found that the women on the pill had lower levels of hormones that play a part in muscle growth and higher cortisol levels.
But another study published in the Journal of Strength and Conditioning, and was co-authored by Mikkonen, that put HC users and non-HC users through a 10-week training program consisting of two days of strength training and two days of running per week, found no significant between-group differences in performance.
Hormonal birth control and athletes: Effects on musculoskeletal system
People on hormonal birth control might benefit from a bit of protection to their tendons and ligaments. For example, during the luteal phase of the menstrual cycle, the ACL is at peak laxity due to an increase in the hormone Relaxin-2. Levels of Relaxin-2 have been found to be significantly reduced when taking hormonal birth control, offering protection from injury.
While ACL injuries are where the majority of musculoskeletal/hormonal contraceptive research has taken place, other studies have shown the hormonal birth control users may also benefit from improved stability (and thus fewer injuries), less severe concussion symptoms, but more instances of injury to the Achilles for unknown reasons.

Hormonal birth control and athletes: Effects on recovery
Recovery is one area where going au naturale may be beneficial. That’s because hormonal contraceptives can lead to more inflammation due to higher levels of cortisol, says certified sports nutritionist Nancy Gomes. This was shown in a study published in the Journal of Applied Physiology, where researchers followed competitive collegiate soccer players for a four month season, comparing women who had been on birth control consistently for at least a year with women who were not. The women on oral contraceptives had significantly higher levels of inflammation and stress biomarkers.
And while there are nutritional interventions that can help with inflammation, Gomes wants to know more about the long-term effects that the increased cortisol levels have on athletes beyond the short-term research being conducted. “It doesn’t speak to what’s happening as you’re doing this every single day, what the accumulation of, perhaps many years, on the pill might be doing to impact inflammation and things like an extended high period of cortisol.”
The authors of the soccer study believe that their findings “corresponded to a potentially reduced capacity for training adaptations and recovery,” among oral contraceptive users.
Gomes points out that it’s extra important that HC users make sure they are eating and hydrating well, as a major, tell-tale sign of RED-S – lacking a period – will not be visible. “To some degree, if somebody is on the pill constantly–the withdrawal bleeding is not a real period, so you can’t get a clear indication of whether somebody’s under-eating is causing any issues. So really you have to examine their dietary intake and try to understand how they’re doing and is it enough for the activity that they’re doing.”
RELATED: Despite Increased Awareness, RED-S Still a Major Problem in Endurance Sports
How should I change my training while on hormonal contraceptives?
Endocrinology research scientist Zane Hauck, Ph.D., notes that triathletes on birth control have a bit of an advantage in dealing with hormone levels that are relatively flat. “Generally, you don’t have to try to find races that fit in your cycle better. You don’t have to change your training regimens, you can kind of do the same training regimen because you’re not having this cycle of hormones,” he says.
For example, with the rise of estrogen in the follicular phase of a natural menstrual cycle women, comes a hampering of the ability to store carbohydrates. “Especially in triathlon, you need such a good storage of energy to kind of last for the entire event,” says Hauck.
On the flip side though he notes that the estrogen spikes in a regular menstrual cycle are beneficial for things like strength training and women on hormonal birth control would miss out on those.
There are a few things HC users can do to give themselves a bit of an edge. Stacy Sims, Ph.D., leading sports nutritionist and physiologist, wrote in a column in 2020 that in order to mitigate impacts birth control might have on training and racing, athletes should increase their protein and anti-inflammatory food intake and incorporate plyometrics and multi-directional jumping into their strength training routine to improve bone density.

Thinking about stopping your hormonal contraceptives for athletic performance?
If you are concerned that hormonal contraceptives might be impacting your swim/bike/run performance, you have a lot of factors to consider.
Instead of going off of them entirely, you can speak with your health care provider and determine if there is another HC out there that might be a better fit. “I think it is important to remember that hormonal contraceptives are excellent tools for physically active women, but sometimes finding the ‘right’ hormonal contraceptive can take time,” says Mikkonen.
If you want to get off of HCs completely, then it’s time to weigh the pros and cons. Think about the reasons you started taking that specific hormonal contraceptive–something that’s easy to forget about if you’ve been on it for a long time. If it helps ease severe menstrual symptoms that might keep you doubled over for several days, then staying on it may be better for your training ultimately. Or if preventing pregnancy is key, are there non-hormonal options that will fit your lifestyle?
If you’re not sure what kind of effect birth control is having on you, consider tracking your symptoms with a convenient app like Planned Parenthood’s Spot On Period Tracker. (Note: The app uses inclusive gender neutral language and allows users to interact without creating an account, if privacy is a concern).
Hauck recommends triathletes get a standard hormone profile test done to test their levels of testosterone, estrogen, progesterone, cortisol, and SHBG (sex hormone binding globulin). “Essentially, anytime your hormones are low, it’s going to affect your endurance,” he says. Understanding your hormone levels can help you and your health care provider make an informed decision about your birth control.
If you’re in the middle of a training cycle, it’s best to wait until the off-season to switch up your birth control regimen.
Alternatives to hormonal contraceptives
| Type | How it works | Effectiveness (w/ correct use) | Possible side effects |
| Copper IUD | Immobilizes sperm | 99% | Cramping after insertion |
| Condom (external and internal) | Creates a barrier | 85/79% | |
| Diaphragm | Creates a barrier | 88% | Bladder infections |
| Spermicide | Immobilizes sperm | 71% | Urinary tract infections Allergic reactions |
| Vaginal gel | Changes vagina Ph | 86% | Urinary tract infections Yeast infections |
| Natural family planning | Tracking fertility | 76-88% | |
| Vasectomy | Sterilization | 99% | Temporary pain and bruising |
| Tubal ligation | Sterilization | 99% | Changes to period Risks related to surgery |
“I would encourage women who are not satisfied with their current hormonal contraceptive to find a knowledgeable health care professional with whom they can share their concerns and their goals–switching formulas or delivery methods can make a big difference for an individual,” says Mikkonen.
The bottom line on hormonal contraceptives: As an athlete, you get to have the final say in deciding what is best for your body, your training, and your life. Multiple options are available for those who are in need of a contraceptive method, and choosing one (or choosing to go without) is a decision that should be made with all goals in mind.