The Modern Art Of Recovery
Gone are the days of simplistic recovery tools. Innovative techniques are taking over contemporary rehab and quickly gaining in popularity.
This article was originally published in the July/August 2012 issue of Inside Triathlon magazine.
Sports medicine has come a long way since the days of menthol-soaked training rooms, filled with runners with taped shin splints and soccer players with iced sprained ankles.
In triathlon, advances in sports medicine are being adopted with great zeal, as triathletes attempt to master what many people call triathlon’s fourth sport: recovery.
The sport’s elite athletes are usually the first to try out new therapeutic techniques—whether for injury rehabilitation or routine recovery—often in the hope of gaining a competitive edge or extending a career. These techniques—if the elites find that they work—also quickly trickle down into the age-group ranks.
Indeed, just a few years ago “recovery” meant nothing more than a massage or a protein shake. Compression gear was confined to the medical industry and anyone wearing hip-to-heel inflated moon-boots would raise an eyebrow. Now, recovery boots are yesterday’s news. Intricately patterned kinesiology tape decorates mountains of skin at any swim start. And muscles are compressed by the thousands with über-tight socks, shorts, shirts and arm sleeves.
So what’s on the cutting edge today? What are the pros using that, given some time, you might find yourself turning to for recovery? And what will it take for you to get on the cutting edge and try out some of these techniques yourself?
The AlterG
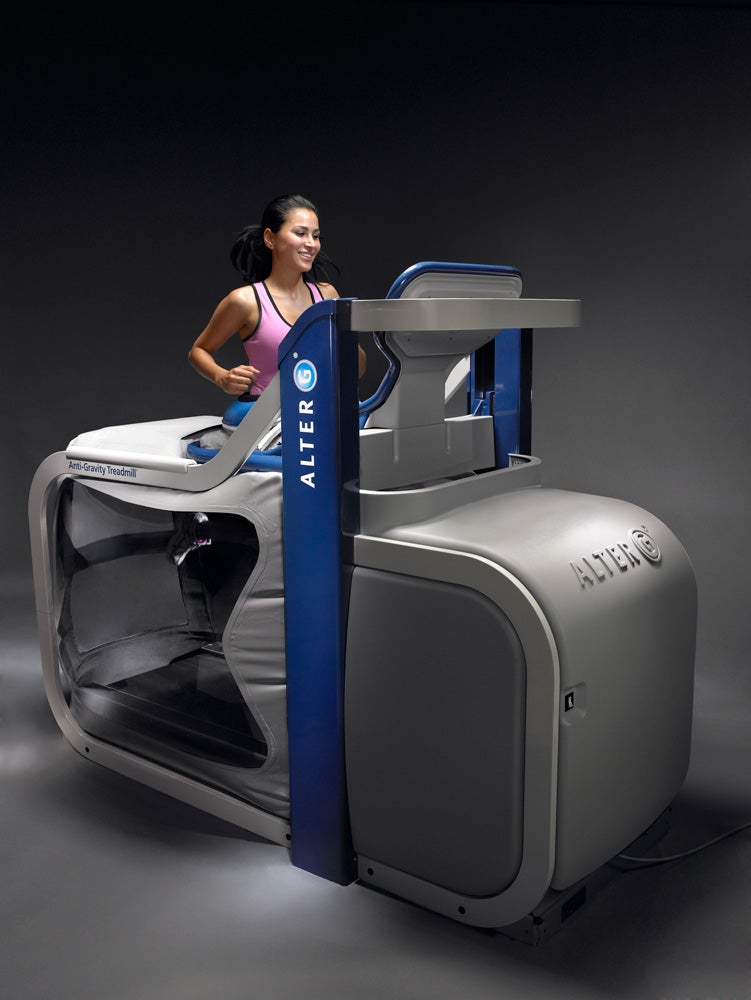
Ever wonder how it would feel to walk—or run—on the moon? The AlterG Anti-Gravity Treadmill simulates that experience. While it resembles a traditional treadmill, it is outfitted with an airtight capsule into which the user is zipped at hip level, wearing lightweight knee-length neoprene shorts. The runner’s weight is calibrated, after which the compartment is pressurized to lift the individual, progressively reducing his weight by up to 80 percent (enabling him to run at a weight as low as 20 percent of his normal body weight). This reduction in weight causes a subsequent reduction in impact, allowing an injured runner to keep running—thus preserving his natural gait and muscle firing patterns—while giving his body an opportunity to heal. Today, elite athletes also use it to get in extra miles at a lower physical cost, or to practice running at a pace they couldn’t manage at full body weight—thus allowing their bodies to experience neuromuscular firing patterns they couldn’t otherwise.
Previously only available to elite athletes, the AlterG’s presence is now growing as more and more physical therapy clinics and chiropractic offices are offering the high-tech treadmill. (The machine costs $32,400 or $75,000, depending on the model.)
“We went to the AlterG because we have a lot of patients who resort to water running or the elliptical machine, but they really are unable to mimic the true run motion,” said Bob Cranny, a Boulder, Colo.-based physical therapist who recently purchased AlterG treadmills for two of his clinics. “Although you’re utilizing the same muscles as running, it’s not in the same capacity. And there are a lot of injuries or issues that people are dealing with—even from a recovery standpoint—where you do want some kind of impact.”
Cranny describes the body as “an incredible adaptive machine.” As long as the stresses on it are consistent and gradual, it will adapt to almost anything. But because water running is completely non-weight-bearing, the body doesn’t get the impact it really needs for active recovery from injury or hard efforts.
“Take a stress fracture,” he explained. “While with your standard stress fracture doctors tell folks to take six weeks off running altogether, we’ve been able to put people—with a physician’s approval—on the AlterG at four weeks at 70 percent of body weight. So they have two weeks of true running under their belt before they go back outside.”
This gives athletes a more gradual build back to full-force running, in addition to minimizing the time lost from training.
“I’ve done a fair amount of water running over the years and I think the AlterG is way better,” said pro triathlete Julie Dibens, a former 70.3 and Xterra world champion. “It’s more realistic, plus I think you get more benefit from it psychologically. In the water I’ve never felt like I was actually running. And anybody that’s done water running would agree that it’s boring as hell!”
The AlterG is equally appealing as a recovery tool, Cranny says, as athletes can use it to gain the mental satisfaction of running yet refrain from inflicting more muscle damage and joint stress on a body that’s already in need of a rest.
And because the AlterG does not entirely eliminate impact, it allows for normal muscle contractions and is therefore more effective in flushing the body’s metabolic waste than non-weight-bearing activities.
Former professional triathlete and elite age-group runner Joanna Zeiger, 41, says the AlterG was instrumental in her placing second overall in the masters division of the 2012 USA Cross Country Championships, only three weeks after she ran the U.S. Olympic trials marathon.
“Between the marathon and nationals I ran on the AlterG two days a week and ran three days a week outside,” Zeiger said. “It was about recovery and trying to get in some speed workouts without the heavy load of running outside. I did all the hard workouts on the AlterG, except for a four-mile cross-country race two weeks after the marathon trials. When I first started off I was running at 80 percent [of my body weight], and I would just build a little more each week so at the end I was running at 90 percent or so.”
If you’d like to try the AlterG for yourself, Cranny says that the time you spend on the device and the weight you run with will depend on your conditioning, injuries and the way they feel during the AlterG session—all variables that should be worked out under the guidance of a professional, he said.
He also cautions against an over-eager need for speed.
“I have seen people become a little overzealous in situations like this,” he said. “Because they’re unweighting themselves, they’re able to run at a pace they normally wouldn’t be able to run, and that can impact them adversely. Their body is not accustomed to the shift in biomechanics due to running at a higher speed.”
As a general rule, runners using the AlterG should run their normal pace. Cranny warns that this is especially true of athletes coming off an injury. They need to progress steadily—not suddenly run faster than ever before. The exception would be the uninjured, non-fatigued athlete.
“Say their maximum pace is an eight-minute mile, and they just want to get a feel for what it’s like to run at a 7:30 pace. That’s fine. It would be like drafting in a pace line on the bike—a chance to get that neurologic feedback of running a 7:30 pace and reeducate those adaptive muscles. But don’t go overboard,” Cranny said.
While the AlterG may not be intended for running at warp speed, it can be an invaluable outlet for the high-mileage runner. Legendary running coach Alberto Salazar is reported to use the treadmill to lessen the load on his long-distance disciples.
“He’ll have them do their two-hour runs at 80 percent body weight,” Cranny said. “So they unload their bodies by 20 percent and they reduce the risk of injury. They’re still getting the physiological impact—they’re still getting the normal running motion—and yet they’re walking away after a two-hour run without all the damage that would normally be done.”
Ins & Outs of the AlterG
BEST FOR | Lower extremity injuries that may benefit from partial weight-bearing (under the supervision of a physician); recovery from intense physical effort
BENEFITS | Promotes active recovery; prevents atrophy post-injury; enhances healing; similar physical and psychological effects as regular running
WHAT TO EXPECT | Feels a bit odd initially, but after a short adjustment period it feels very similar to a traditional treadmill (albeit at your grade school weight)
SIDE-EFFECTS | Body image can be hindered by a post-run return to normal weight!
CAUTIONS | Overzealous use—running too fast on the treadmill or too soon following injury
PROS | Ability to return to running (post-race or post-injury) sooner than with full-impact exercise; precise control over progressive weight bearing, pace and incline
CONS | Running in neoprene shorts; it’s still running on a treadmill
COST | A nominal fee at any facility listed on the manufacturer’s website (with free initial demo)
FIND AN ALTER G | Alter-g.com
SCIENCE SAYS | The benefits of progressive, controlled loading and mobilization of healing tissue and bone are well-documented, as are the adverse effects of keeping injured tissue immobilized. A few studies have been published validating the claim that running on the AlterG helps a runner maintain normal gait and muscle firing patterns while decreasing joint loads. Clinical studies into the specific applications and treatment protocols associated with the AlterG are currently in progress.
BRETT SUTTON’S DIY ANTI-GRAVITY TREADMILL
In the 1990s, triathlon coach Brett Sutton held training camps in Jindabyne, Australia. While there, he created a do-it-yourself—and much cheaper, albeit less scientific—AlterG that anyone with engineering sense could put together. He believes it helped Loretta Harrop, the 2004 Olympic silver medalist, train through several stress fractures.
“We put a pulley in the roof, and I attached a rope to a mountain climbing harness,” Sutton said. “I would be on the end of it and I would take the weight by lifting her above the machine. It was all my guesswork how much we lifted her. I would say it helped her win at least eight World Cups with stress fractures. The new-fangled version I believe would be a terrific tool, but I’ll never be able to afford one.”
Dry Needling
Dry needling, or trigger point dry needling, targets trigger points, or tiny knots that dry needling practitioners say develop in muscles when they are injured or overworked.
“Trigger point therapy has been around for a really long time, but we used to use our hands a lot [instead of needles]. Then it was discovered that if you actually put a needle deep into the muscle you can get a really good response,” said Christine Bell, a Boulder-based physical therapist. Dry needling practitioners use the same needles that acupuncturists use; they tap the needle into the trigger point in the hopes that the muscle will loosen, eventually reducing pain and tightness.
“What happens with a shortened or tight muscle is that it is continually firing,” Bell said. “A chemical is continually released into the motor end plate of the muscle [the spot where nerve impulses are transmitted to the muscle], which makes it fire and keeps the muscle short. That’s a dysfunctional muscle. It can’t contract properly. Dry needling will get rid of the chemical substances in the muscle by producing a twitch response [the release of the trigger point], and it also helps to realign the muscle fibers to restore a more normal length and tension balance. Then it can contract normally, and then you can strengthen it. The muscle not only feels better instantly, but then when you go out and exercise you can actually do it, so you can get stronger.”
Widely practiced in Canada, Australia, New Zealand and Europe, dry needling is rapidly gaining popularity and acceptance in the United States. Roughly a dozen states currently allow physical therapists and chiropractors to dry needle (following proper training), and proponents of the technique are attempting to increase this number.
While most of the evidence in favor of dry needling is anecdotal, case studies cite improvement in a variety of conditions including chronic muscle tightness, piriformis and hamstring issues, patellar tendonitis, Achilles tendonitis and rotator cuff injuries.
One of the earliest studies of dry needling in the treatment of chronic muscle pain was published in 1979 by Karel Lewit, a physician from the Czech Republic and a pioneer of the technique. Lewit reported that of 241 patients and 312 sites treated, immediate relief was felt in nearly 87 percent of locations needled. That is, while some patients experienced no change, the majority felt pain relief ranging from several days to several weeks to permanent improvement.
Ironman champion and Arizona-based triathlete T.J. Tollakson, for example, believes that dry needling helped him recover quickly from recent hip surgery. “One of the drawbacks of the surgery is a super sensitive hip flexor group,” Tollakson said. “[My physical therapist] recommended I try dry needling along with my current rehab and strengthening routine—I’m a huge fan. I believe it aided in an increased healing process of my hip flexor group and allowed me to get back to full training sooner.”
Anyone interested in dry needling should note that the process can be painful.
“The needles pushed through my IT band tended to be some of the most painful ones, along with needles in my psoas and iliacus,” Tollakson said. “I would leave each session walking with a slight limp from being so sore and I developed a few quarter-sized bruises in different injection sites, though most of the needles left no bruising.”
Tollakson said he was quite sore immediately after each session, but improved over the next few days.
Ins & Outs of Dry Needling
BEST FOR | Muscular tightness or imbalance; soft-tissue injuries; back or pelvic misalignment
BENEFITS | Restores proper muscle function, flexibility and range of motion; decreases pain
WHAT TO EXPECT | Sensations range from unnoticeable to painful, depending on the individual, the location needled and the condition of the muscle
RESPONSE TIME | Some degree of immediate improvement; complex or chronic conditions require longer-term treatment
SIDE-EFFECTS | Temporary soreness lasting a few hours to a day or more; occasional bruising
CONTRAINDICATIONS | People taking anticoagulants; people with infection or road rash (needling dramatically increases blood flow); pregnancy (in some instances)
COST | Comparable to a physical therapy office visit
TIPS | As with deep-tissue massage, post-treatment drink plenty of water and avoid being completely sedentary in order to increase circulation and flush out released toxins
FIND A PRACTITIONER | Physical therapy website Kinetacore offers dry needling education and provides a link to certified therapists nationwide: Kinetacore.com
SCIENCE SAYS | Several studies of dry needling find the technique effective in the treatment of muscle trigger points; however, the consensus is that controlled trials would be necessary to determine whether the results are conclusive or a placebo effect.
Extracorporeal Pulse Activation Technology
“It feels like a million bee stings!” said professional triathlete and Ironman champion Linsey Corbin of extracorporeal pulse activation technology (EPAT). “It’s almost like a jackhammer, but it has a blunt end.”
EPAT is a therapeutic treatment in which sound waves are delivered to the injury or pain site through the skin with a hand-held applicator. Its origin is in extracorporeal shockwave therapy, or ESWT, a common practice used by urologists. According to practitioners, EPAT breaks up scar tissue, stimulates the metabolism, increases circulation and fast-tracks the body’s natural healing process.
“ESWT has been available since the early 1980s for the treatment of renal stones and biliary stones [kidney and gallstones],” said John Ball, a chiropractor based in Phoenix who administers EPAT. “The shock waves break up solid structures into smaller fragments and allow for the spontaneous passage of the stones.”
EPAT is believed to work in a similar fashion on the scars and calcium deposits that develop after an injury. “EPAT disrupts these calcific deposits and scarring. It loosens the soft tissues and promotes reabsorption of calcium, thereby decreasing pain and improving function,” Ball said.
Because EPAT is an emerging technology, there’s still much to research on its optimal dosages, response times and overall effectiveness.
What is known, however, is that elite athletes from all over the country travel to Phoenix to visit Ball and receive treatments using EPAT.
These athletes include Ironman champion Chris Lieto, who had an Achilles injury that Ball says he treated successfully; 2012 elite cross-country national champion Sara Hall, who received therapy for hamstring and hip issues; professional triathlete Rachel Joyce, who saw Ball for hip and groin injuries; two-time 5,000 meter national champion Lauren Fleshman, who received treatment for a foot injury; and Ironman champion Linsey Corbin, who saw Ball for a hamstring injury.
“I ran around like crazy trying to find a solution. I tried acupuncture, dry needling, crystals, PT, ice, rest, natural supplements, strength imbalance work. I saw an osteopath, a naturopath, people in Oregon, Tennessee, Montana—you name it. Nothing was working for me,” said Corbin, who lives in Montana but trains in Tucson when the weather is particularly cold.
She eventually found Ball through a referral from Olympic marathoner Ryan Hall. Whereas previous practitioners had focused on Corbin’s lower hamstring where she felt the pain, Ball went straight to her hip and gluteal region.
“Basically his theory is that as athletes, we’re building up scar tissue over time,” she said, “layering Band-Aid upon Band-Aid upon Band-Aid, but what we want is to have our muscles smooth like putty. He went in with the EPAT machine to clear up all the junk and scar tissue built up in my hip area, which immediately released the tension on my hamstring. It was like I was a free woman again!”
She says he had her running pain-free within a day.
“I stayed in Phoenix for a week on my first visit in June [last year]. I would see him a few times a day,” said Corbin. “I’d go for a run, tell him where I had pain, he’d treat me and I would leave. I’d run, he would evaluate what was tight or restricted, treat the area and I would leave. Again—run, treat, repeat.”
Corbin returned home to her regular training routine, yet paid a follow-up visit to Ball in July 2011, this time for four days, to address lingering scar tissue. She spent an additional three days working with him prior to the 2011 Ironman World Championship 70.3, where she placed third.
“After that I was back to 100 percent of my range of motion and health,” Corbin said.
Ins & Outs of E.P.A.T.
BEST FOR | Treatment of soft-tissue injuries including plantar fasciitis, numerous forms of tendinosis and acute and chronic muscle pain
BENEFITS | Disrupts scar tissue, stimulates metabolism, increases circulation and accelerates healing of injured tissues, resulting in increased range of motion and decreased pain
WHAT TO EXPECT | May feel moderately unpleasant or uncomfortable
RESPONSE TIME | Most conditions respond within 3–4 treatments spread at one-week intervals; chronic conditions may require more intensive treatments, whereas intermittent treatment can aid recovery
SIDE-EFFECTS | Potential for temporary local tenderness or mild swelling
CONTRAINDICATIONS | People with uncorrected bleeding disorders or bone tumors; pregnancy; recent use of steroid injection
COST | Varies depending on treatment and type of medical office, ranging from $95 per single treatment to $750 for three-pack series
FIND A PRACTITIONER | Approximately 500 M.D.’s, D.O.’s, D.P.M.’s and D.C.’s nationwide currently use EPAT; contact CuraMedix directly for referral to a practitioner near you: Curamedix.com
SCIENCE SAYS | Research in support of ESWT (and ESWT-derived techniques such as EPAT) as a treatment for musculoskeletal conditions is limited and primarily focused on plantar fasciitis and chronic tendinitis.