Anatomy of a Stress Fracture

(Photo: Getty Images)
When it comes to running or triathlon-related overuse injuries, stress fractures (or bone stress injuries) are often the most dreaded, for good reason, as they can quickly shut down a season. They seem especially prevalent in the tri world this year, as everyone from Lucy Charles-Barclay to Linsey Corbin have been hit with stress fractures. But it’s not just the pros who are affected – up to 30% of all running-related injuries are bone stress injuries, sidelining age groupers for weeks and months. So what are stress fractures, and how can you avoid getting one?
RELATED: Why Are So Many Triathletes Getting Injured This Season?
What are stress fractures?
Bone stress injuries are considered overuse injuries that occur when repetitive mechanical loading on the bone causes accumulative microdamage at a rate that outpaces bone remodeling and repair, leading to breakdown and microfracture. Normally, initially with loading activity, cells called osteoclasts break down bone. If rest is sufficient, cells called osteoblasts then repair the damage and strengthen the bone. If not, osteoclasts outpace osteoblasts, and bone weakening occurs.
Stress fractures vs. stress reaction
Bone stress injuries exist across a continuum. In early stages, microdamage accumulates and pathological changes may be occurring, but the athlete might not yet be experiencing symptoms. If loading continues to outpace remodeling, the injury can develop into a stress reaction, which features edema (swelling) within the periosteum (outer lining of the bone), or bone marrow (inner filling of the bone). Stress reactions can progress into stress fractures, where a clear fracture line is also visible on imaging with disruption to the bone’s dense outer shell, called the cortex.
Where do stress fractures occur?
Not surprisingly, most bone stress injuries in runners and triathletes occur within the lower limbs. The tibia, or shin bone, is typically the most common location with the metatarsals, femur, navicular, fibula, and sacral bones following behind. The lumbar spine or pelvis may also be affected. The long bones (tibia, femur, fibula) tend to be the most affected in distance runners due to loading patterns associated with rearfoot strike patterns, while the forefoot strike patterns associated with higher-velocity running in shorter distance runners tend to load the foot bones (metatarsals, navicular) to greater degrees. Individual biomechanics and loading patterns vary, though, so bone stress injuries need to be considered for all areas.
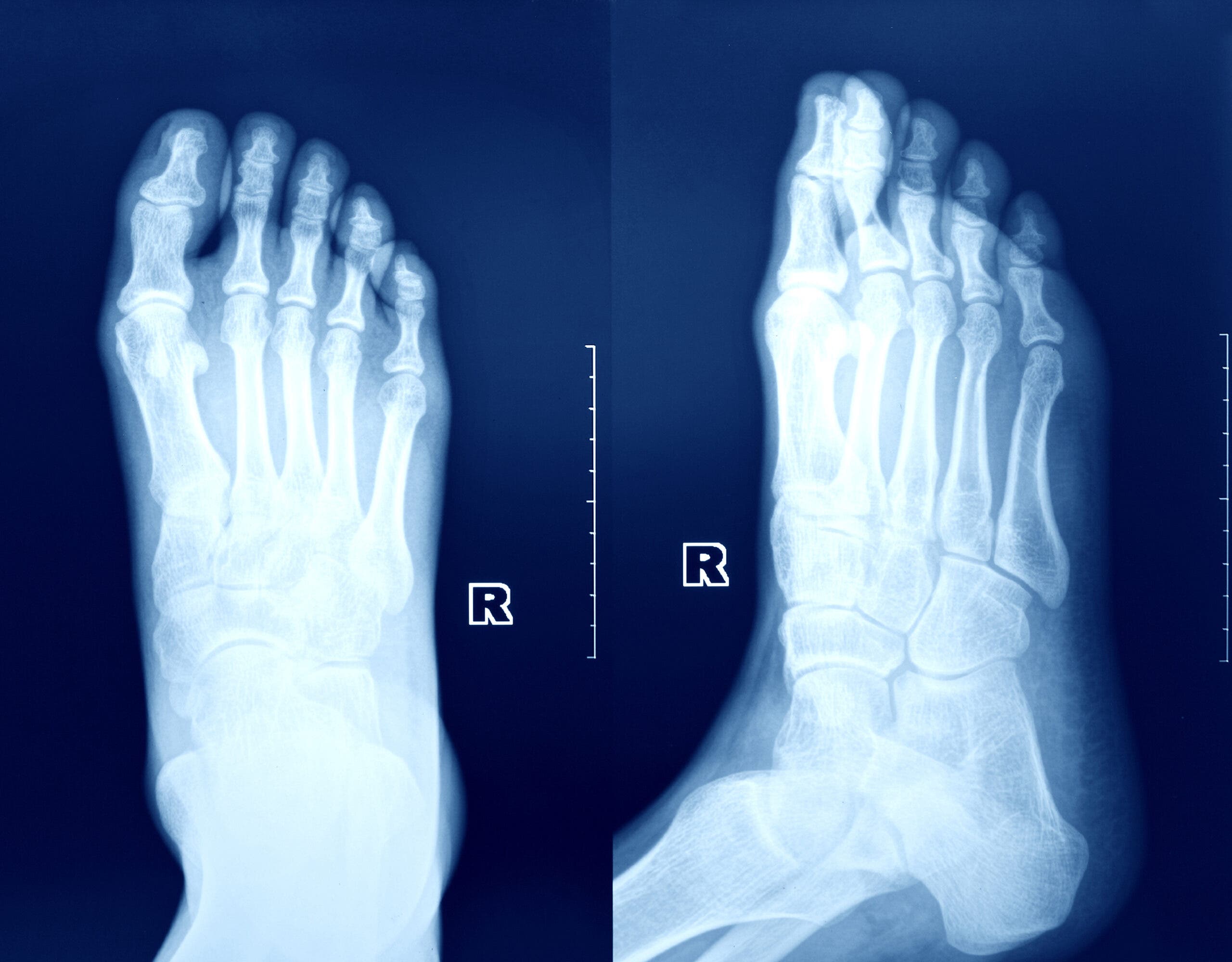
Risk factors for stress fractures
Exacerbating risk factors for bone stress injuries can be classified as intrinsic (internal athlete characteristics), or extrinsic (factors external to the athlete). Intrinsic risk factors typically relate to the ability of an athlete’s bones to resist load, and anatomical or biomechanical characteristics.
Factors that may predispose an athlete to bone stress injury via weakened bones include genetics, certain metabolic bone disorders, high cortisol levels, some medications (namely, corticosteroids) low vitamin D and calcium levels, and (a big one in the triathlon and distance running world), low energy availability, where caloric intake does not match expenditure.
RELATED: Despite Increased Awareness, RED-S Still a Major Problem in Endurance Sports
Females are at higher risk than males, particularly females with a later age of first menarche, and irregular menstrual cycles or absent periods. Low testosterone levels in males can also be a risk factor. Unfortunately, when it comes to stress fractures, many athletes won’t be one and done: previous history of bone stress injury is a strong risk factor for a future one.
Certain anatomical and biomechanical factors that may alter bone loads have been linked to bone stress injury risk, including leg length discrepancies, flat or high-arched feet, and smaller calf muscle girth. Biomechanically, runners with knees that tend to collapse in during midstance or higher loading rates at initial contact (as in, those who over stride) may be at higher risk, as well.
Extrinsically, many training-related factors have been proposed to contribute to bone stress injuries. Predictably, they most often develop after increases in training, particularly running load. Higher volumes cause more bone loading cycles, while higher speeds increase forces on the bones. Additionally, as muscles fatigue, their ability to attenuate shock decreases and form changes occur, leading to higher strains being transferred to bones. As for other factors, evidence about running surfaces and footwear is overall mixed, but some studies have shown increased risk associated with harder training surfaces and worn running shoes. Interestingly, while higher training loads increase bone stress injury risk, longer histories of physical activity may be protective against them, as bones may have strengthened in response to chronic loads over the years.
How to diagnose a stress fracture
Bone stress injuries are most successfully treated they are detected early. What might raise suspicion? Initially, symptoms may be vague and easy to confuse with other, less sinister pathologies. Pain most often during activity, especially running, that does not abate as the run progresses, is usually the earliest sign, followed by pain that persists after activity or with any weight bearing, and eventually, at rest or at night as well. In certain areas where the bone is more superficial (shin, foot), a localized area of tenderness over the bone is present, while deeper injuries (i.e. to the femur) may cause more diffuse pain.
Several quick self-tests can help point to a bone stress injury. The Single Leg Hop Test, which is performed exactly as it sounds, has shown high success with self-diagnosing bone stress injuries. Essentially, pain upon landing impact may suggest a stress injury in lower extremity bones. The Fulcrum Test, which involves placing a forearm under the questionable thigh, pressing down on the knee, and assessing for pain is useful for identifying potential femoral bone stress injuries. Self-diagnosis is difficult, though, and imaging will be needed to be certain.
RELATED: Which Provider Should I See For My Injury?
How long does it take to heal a stress fracture?
If you think you might have a bone stress injury, stop high-impact, provocative (namely, running) activities, and call your doctor – you can’t “train through” a bone stress injury. Often, x-rays are the first imaging test performed, although they have low sensitivity for detecting bone stress injuries, as only more advanced injuries with distinct fracture lines or calluses will be seen. Bone scans are sensitive to detecting activity in bones, but are unable to directly visualize the degree of injury. MRIs, then, are considered to be the gold standard for imaging bone stress injuries, as they can show periosteal reactions, bone marrow edema, and fracture lines, and can help to determine the severity of the injury. Bone stress injuries can be assigned “grades” based on MRI findings, which can assist with determining overall prognosis and healing time, as well.
Healing time and the degree of training and activity restrictions for bone stress injuries vary based upon the location and severity of the injury. Certain areas where bones are either under high tensile stress and/or have poor blood supply are considered to be “high risk”, meaning they are prone to displacement, delayed healing, or non-union. These areas include the femoral neck, the anterior tibia (front of the shin), the medial malleolus (inner ankle bone), the kneecap, and, in the foot, the navicular bone, the sesamoids, and the base of the fifth metatarsal. Lower risk areas include the lower, posterior portion of the tibia, the fibula, and the rest of the metatarsals. Injuries involving the pelvis, sacrum, and femoral shaft tend to fall somewhere in between. A review across all types of bone stress injuries found that average return-to-play time was about seven weeks for the lowest grade of injury, 10-12 weeks for moderate grades, and 14 weeks for the highest grade, where fracture lines are present. So, in general, plan on 6-8 weeks to heal those low-grade, low-risk injuries, and anywhere from 4-6 months for the high-grade, high risk ones. Unfortunately, some high-risk fractures do end up requiring further medical intervention (surgical fixation, bone stimulators, medications) to resolve, leading to more delays in healing time.
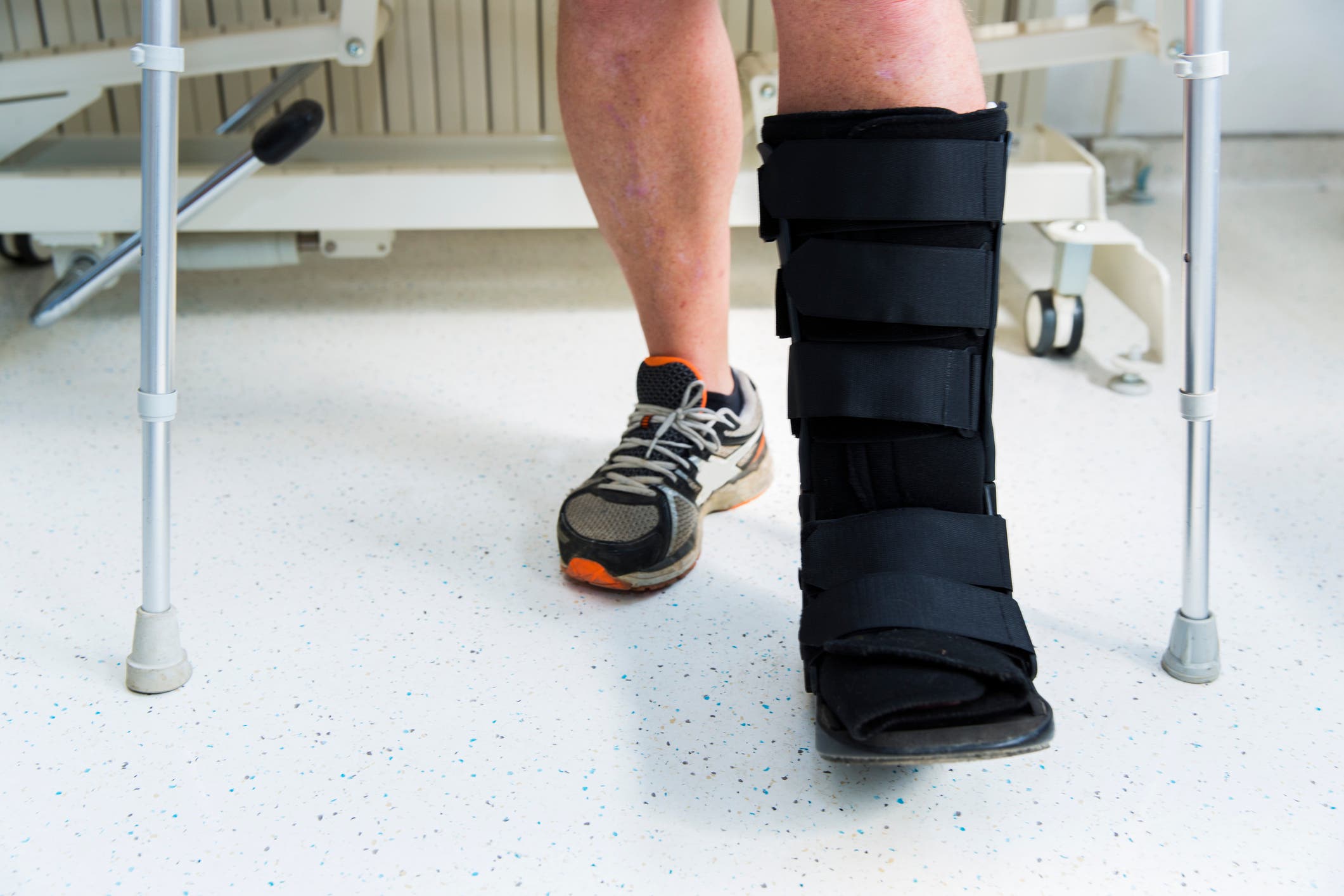
Can I train with a stress fracture?
The first line treatment for bone stress injuries is activity modification, and, in some cases where standing and walking are provocative as well, non- or protected weight bearing. Universally, high-impact activity (as in, running) will need to be avoided until the injury is healed, and the area is pain-free. Otherwise, the degree of activity restriction will depend upon the grade and location of the bone stress injury. Low-grade, low risk fractures (i.e. a tibial stress reaction) may only require restriction of running, while swim and bike training can be maintained.
For moderate-risk injuries, or low-risk injuries at higher grades, biking may need to be limited, as it can still put strain on bones, despite the lack of impact, while water-based training (swimming, water running) can continue. In any case, pain should be used as a guide-increased pain during or after activity indicates too much bone loading for the stage of healing. High-risk fractures often put a full halt on training, though. Muscle tensions or any movement at the fracture site are risky, meaning that total rest is needed, likely including immobilization and/or non-weight bearing (hi, crutches!) on the affected limb.
A further consideration is energy balance. When an energy deficit was involved in the development of the bone stress injury, rebuilding the body’s reserves and reversing the deficit should be prioritized over trying to be a cross-training hero, and digging the hole deeper. Other precipitating factors (vitamin D deficiencies, menstrual irregularities) should also be addressed by appropriate medical professionals prior to resuming training, and biomechanical and strength deficits should be evaluated. Remember, too, that the healing timelines above are meant to be guidelines for bone healing, not for “jumping right back into normal training”-as a rule of thumb, plan on a week of a gradual return to full training load for every week it takes for the bone stress injury area to become pain-free.
RELATED: Everything Endurance Athletes Need to Know About Vitamin D
Bone stress injuries, unfortunately, occur frequently in triathletes and runners, and are a source of much missed training, racing, and physical and emotional pain. With proper identification of risk factors, early detection, training modification, and gradual return to activity, though, they can be successfully overcome, or – even better – prevented in the future!
RELATED: An Injury Guide For Triathletes
Jennie Hansen is a physical therapist, Ironman champion, and USAT Level 1 triathlon coach with QT2 systems. Hansen has a background as a collegiate and professional runner, as well as a number of professional triathlon podiums. She has been in the sport for over a decade.