Understanding the Science Behind Glucose Monitoring
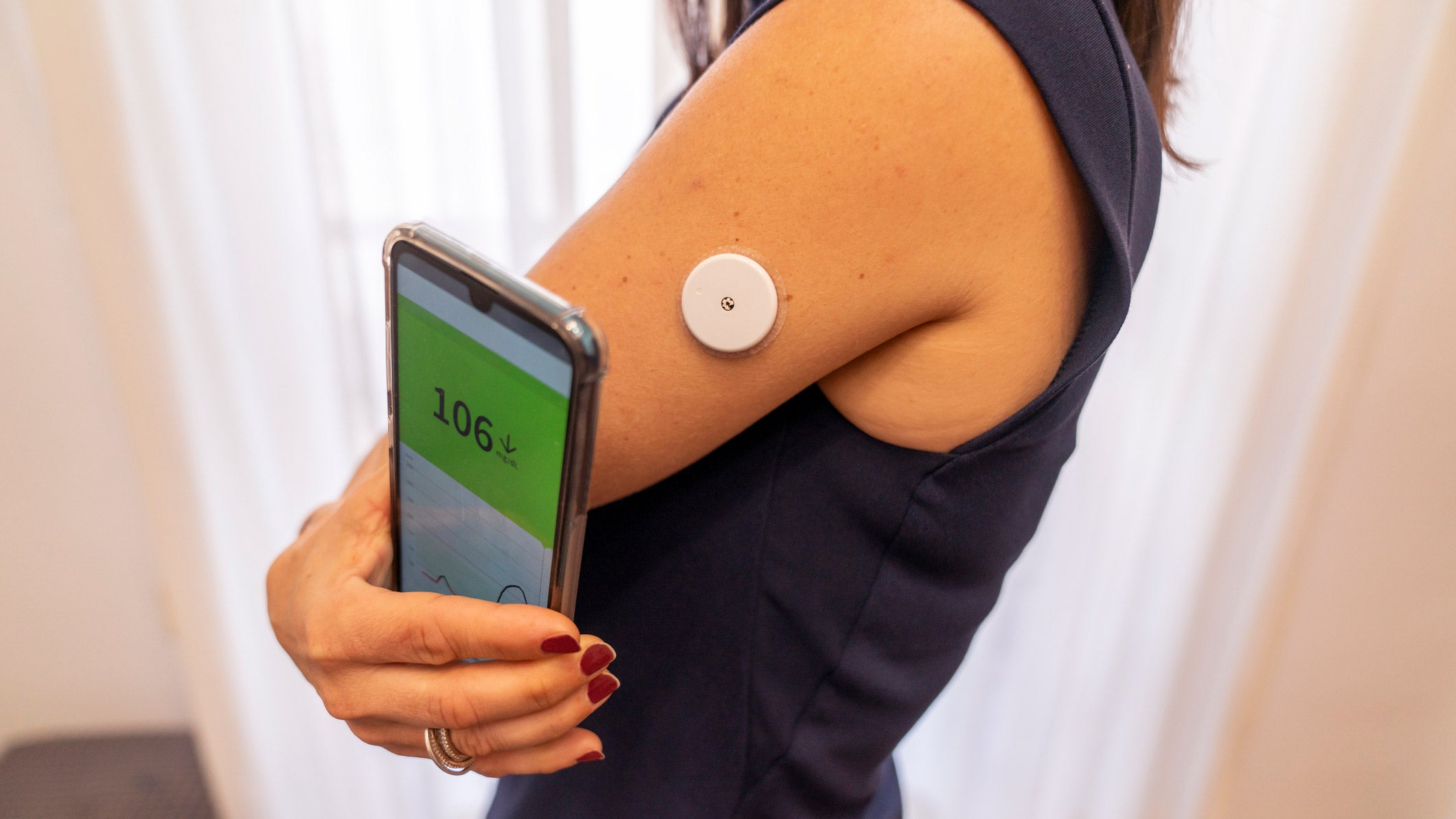
Glucose monitoring seems to be all the rage at the moment. You can’t help but notice those little white discs firmly implanted on the triceps of professionals and amateurs alike. No, they’re not diabetics. They are part of a growing number of athletes seeking an edge through technology and biohacking in the form of a better understanding of fueling requirements based on their glucose levels. The small sensors—about the size of two stacked quarters—can be scanned discreetly with a compatible smartphone, even through clothing, and some can be connected to an external device via Bluetooth.
To date, the two major options for athletes are the Supersapiens and Levels platforms. Triathlete took a deep-dive into the Levels platform before and compares the two here. While both products are still being fine-tuned, the idea behind glucose monitoring is to use real-time data to spot spikes or drops in blood sugar—and adjust your diet or activity accordingly.
What we’ll be looking at in this article is why this matters, the science behind blood glucose, and what the short-comings are of the current options. If you want to see a detailed comparison of the two devices and platforms currently on the market, then check out: Two New Glucose Monitoring Devices—Why, How, Which is Best?
RELATED: Reviewed: Levels Real-Time Blood Glucose Monitoring
Why Do You Want to Measure Your Blood Glucose Anyway?
First, why should we monitor blood sugar levels? From a health perspective, it’s recommended in order to avoid large spikes in blood glucose and to minimize risk of cardiac disease and reduce the risk of developing conditions such as metabolic syndrome and eventually diabetes. From an athletic perspective, creating stability in your blood glucose could reduce cravings and help to stabilize food intake, thereby reducing overall caloric intake (if weight loss is one of your main goals). It also helps in avoiding bonking by monitoring real-time blood sugars and optimizing the potential for exact feeding strategies.
So how do the current tech and science behind these monitoring systems work?
Real-Time Continuous versus Intermittently Viewed Glucose Monitoring
Both Levels and Supersapiens use a technology that was previously restricted to diabetics. They rely on a sensor that measures interstitial fluid glucose levels. The current Levels device uses Abbott’s Freestyle Libre sensor, while Supersapiens uses a different sensor made by Abbott, called the Libre Sense Glucose Sports Biosensor. It is effectively the same device but the Libre Sense has some modifications aimed more at the active user.
It is important to note that the Levels Freestyle Libre sensor is not a real-time monitor but rather an intermittently viewed monitor (or flash glucose sensor). That means it stores the data and then requires the user to scan the device with a phone. Supersapiens’ Libre Sense, on the other hand, relies on Bluetooth to transmit real-time data to a smartphone and potentially then to another device for viewing (it also stores data for when the connection is not active). This is important because only a real-time glucose monitor can truly warn the user of an impending hypoglycemic or hyperglycemic event. For a diabetic, the real-time alarm is obviously important—but this is also where athletes may be looking to gain live information relating to performance. Both real-time and intermittently viewed monitors can provide information about time in zones, variability in glucose readings, and can display graphical representations of glucose trends. The ability for a sensor to connect, in real-time, to wearables is a big deal to the endurance athlete and also to nutritionists working with athletes to deliver precise fueling recommendations based on “current events.”
What We Measure When We Measure Blood Glucose
Blood glucose measurements are critical to effective diabetes management. However, the use of such measurements for athletic performance has not been studied—and so all the technology and subsequent discussions are based on what is known for diabetic patients.
Venous Blood Glucose
Traditional testing of glucose has been performed through blood testing. This is either via a venous sample or via fingertip capillary testing. Venous samples can be performed by your doctor via a blood collection in a fasted state. The measure of blood, then, is a direct measure of glucose in your blood at that moment in time. It indicates your glucose levels at rest and after a fasted period. This is one of the pitfalls of venous draws—it cannot be completed very often and is therefore not particularly practical for many people, especially athletes when relating it back to performance rather than purely health.
Capillary Blood Glucose
Capillary testing is a finger prick style test using a puncture device, a strip, and a sensor unit—as is common with diabetics. The advantage of this over venous blood samples is that it can be performed multiple times per day at the convenience of the user. It does, however, involve sticking your finger, squeezing the blood onto a strip, and assessing the sample. The accuracy of this reading will depend on the analysis unit being used. The accuracy of these units can vary from 3% to 15% when compared to venous measurement. While 15% might seem like a lot, it is the trends over time that are most important to the user.
HbA1c (glycated haemoglobin)
A doctor can request to test your HbA1c (glycated haemoglobin). This marker is considered the gold standard for blood glucose assessment. This marker does not necessarily need to be completed in a fasted state, although it is often measured at the time a fasted blood draw is done. This marker represents the average amount of sugar (glucose) in your blood for the past 90-120 days and is reflected as a percentage. A reading of less than 5.7% is considered normal; 5.7 to 6.5% is considered pre-diabetic. I will often request this test in blood panels with all the athletes I work with as a baseline measure for glucose control. When viewed with other markers, including iron markers (haemoglobin, iron, ferritin), a better overall clinical picture can be developed.
HbA1c is a measure of glucose control, yet it does not reflect day-to-day glycemic control for the individual. Rather, it gives an overall average shown in the percentage. This has limitations when relating it to health parameters surrounding hypo- and hyperglycemic events as it will not tell you if you had any of these events. It is just a single number indicating your glucose as a percentage over that period. There is also an issue with altered readings based on iron levels, a common problem with endurance athletes, so the value being represented may be underreported due to low hemoglobin levels. HbA1c refers to glycated hemoglobin—a combination of hemoglobin and glucose. The underreporting of values is possible if your hemoglobin is low because that is what your glucose is attached to, so if you have low hemoglobin due to anemia or other iron-related issues then your HbA1c will be reported as low.
Interstitial Fluid Glucose
The intermittently viewed glucose monitors being used commercially to measure performance benefits don’t measure HbA1c. They use technology that measures interstitial fluid glucose concentrations rather than blood glucose. Interstitial glucose values are determined by the rate of glucose diffusion from blood plasma to the interstitial fluid and the rate of glucose uptake by subcutaneous skin cells. As a result, interstitial glucose levels can be affected by factors such as insulin levels, blood supply to the area, and potential permeability issues caused by nerve stimulation. The measurement of glucose in the interstitial fluid will differ from venous blood draw with ranges of 11-16% being described in the literature. When you factor in the differences between venous and capillary measurements it is important to acknowledge that these numbers will not be of clinical grade accuracy. This is not to say the numbers are not accurate, but it is worth flagging as a consideration. The accuracy of measurement error has been shown to be stable across a 14-day period, so you can at least be assured that while the reported numbers may not be as accurate as a venous draw, they will be accurate for you and what is being reported. The reality is that the difference is unlikely to make any change in decision making, such as requiring an urgent feed or not. The importance of this is that when viewing the numbers and data, like all data, it is important to focus on the trends and patterns that are viewed over a broader period of time. Like the HbA1c reading that provides a picture of your blood glucose over 90-120 days, the readings that you will get from the device will provide insight into what foods provide continuous large spikes (for me, for example, it is chickpeas and white rice) and detailed knowledge of how prolonged exercise affects your glucose levels and the foods that can elevate levels when required.
Not All Blood Glucose Is Created Equal
Unit Placement
The use of continuous glucose monitors and intermittently viewed glucose monitors is popularized due to the reduced need for capillary (needle finger stick) readings. Not having to draw blood four to 10 times a day is certainly an attractive prospect. One consideration, though, should be the placement of the sensor. Freestyle Libre advises placing the sensor on/around the tricep. It seems some people have experimented with alternative sensor placements, such as the thigh and abdomen, due to the need or want to conceal it, but this can further affect the reliability and validity of the readings.
It’s Complicated
In short, the science behind these units is pretty complicated. The simplicity of what you are getting is very appealing. The user has at their fingertips a value that could, in theory, be used to monitor blood glucose levels to optimize health and performance. The accuracy of the actual measurements could be debated, yet what the absolute values may represent is very interesting. It could be argued that the real value will be once the individual user has collected enough data to better understand how different foods affect their readings. With this knowledge and then subsequent analysis of sessions, “performance zones” can be established for the athlete to know what is optimal for them to achieve the very best results. These zones could then be invaluable to nutritionists and coaches to better refine carbohydrate fueling strategies. It opens up a lot of questions relating to carbohydrate feeding recommendations and whether or not the peak numbers of 90-120g of carbs an hour are required for all athletes to strive for. Going forward, it will be interesting to see how this technology develops, and, as we learn more about how best to use it, what this translates to in terms of refining nutritional strategies for athletes.
Scott Tindal is a performance nutrition coach with 20 years of experience working with pro and amateur athletes. He has a Masters degree in sports medicine and a post-graduate diploma in performance nutrition. He is the co-founder of FuelIn, an app-based personalized nutrition coaching program.